Childbirth through assisted reproduction and IVF is increasingly common in modern society. The process can be costly and there is also risk to the female partner. 60% of infertility is due at least in part to male factors and with modern microsurgical reconstructive techniques some of these may be repaired to allow natural conception.

Although intended to be a permanent procedure, circumstances can change and a vasectomy reversal procedure is available to men who wish to father children naturally after vasectomy. It is estimated that 2-6% of men seek reversal after vasectomy.
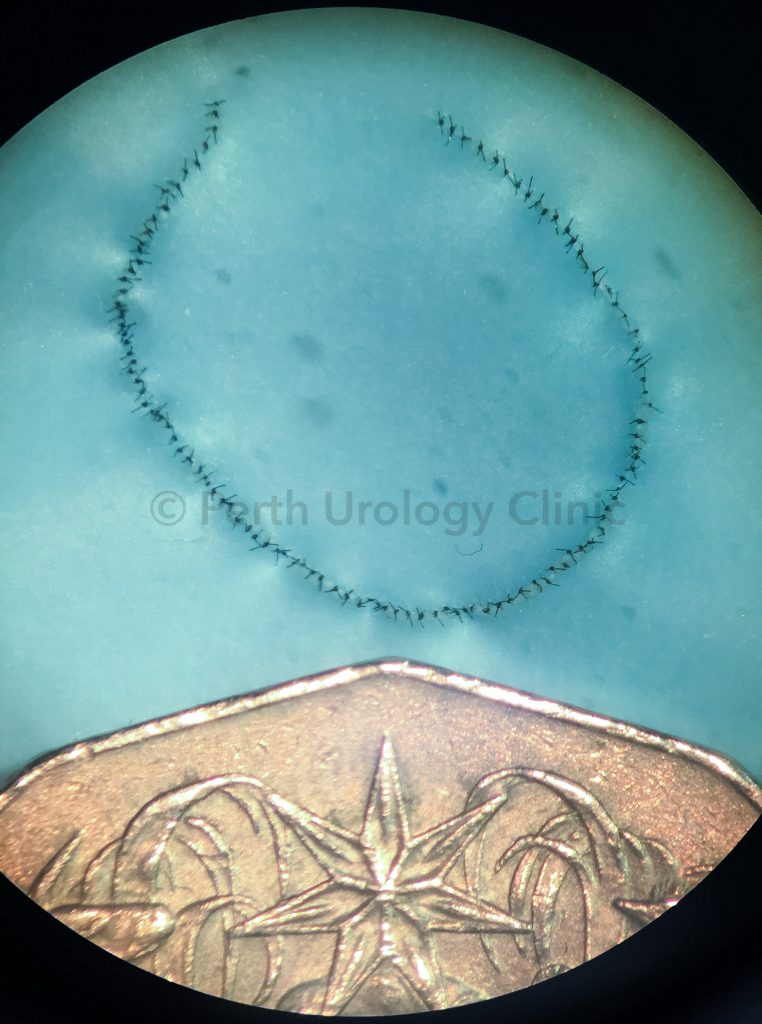
The vasectomy reversal procedure relies on accurately rejoining the cut ends of the vas deferens (vaso-vasostomy), the inner surface of which measures only 0.3mm in diameter. A microscope or surgical robot is used to perform this delicate work with precision, using a multilayer microdot technique.
After the procedure, patency rates of the vas can be upward of 90%. The natural pregnancy rates following a vaso-vasostomy are over 50%.
Even if pregnancy is not able to be achieved the male partner after vasectomy reversal has the benefit of being able to provide a semen sample for IVF without the need for a testicular biopsy.
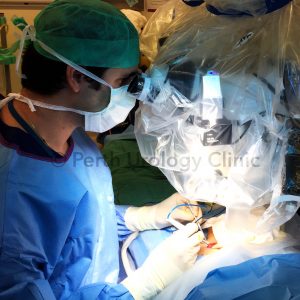
Blockage of the vas deferens may be irreversible, or there may be blockage further upstream as a result of infection, inflammation or previous testicular surgery.
In this case an option is to attach the cut end of the vas deferens to the epididymus, which is next to the testicle and stores the sperm before they drain into the vas. This is called a Vaso-epididymostomy and is the most delicate and complicated technique performed by male infertility microsurgeons. The tubules within the epididymus are tiny compared to the vas lumen which itself measures only a fraction of a millimeter.
Sperm returns to the semen in between 50 and 90% of cases and pregnancy is achieved in 10-50% of cases. At the time of vaso-epididymostomy sperm may be taken for cryopreservation through either epididymal aspiration or testicular biopsy depending on the patients wishes.
In men with no sperm in their ejaculate (Azoospermia), a systematic microsurgical exploration of the testicle has a higher rate of sperm retrieval than random biopsies. Micro TESE can be used to find sperm in men who have had multiple previous negative testicular biopsies.
In men with Azoospermia, sperm production within the testicle may still occur in small patches that are unlikely to be sampled with random biopsies. During Micro TESE the testicle is completely explored using a microscope and areas of sperm production can be precisely targeted and sampled. Because of the precision of the technique there is less testicular tissue removed and less trauma to the testicle than with random biopsies.
Perth Urology Clinic is proud to offer this technique in association with local fertility clinics to give men with Azoospermia an alternative to donor sperm or adoption.